With Low COVID-19 Numbers, Northeastern States Not Doing Enough To Test, Prepare

Guwahati: On April 27, 2020, the northeastern states of Manipur, Arunachal Pradesh, Tripura and Nagaland were declared “COVID-19 free,” Assam, Meghalaya and Mizoram had 20 active COVID-19 cases and Sikkim has no cases. However, in the eight days since, 40 new cases have been detected in Tripura and eight in Assam, where there is a fear of community transmission after the government was unable to trace the source of four cases, and fear of a resurgence of the disease as migrants return.
The region is not testing enough and states’ healthcare systems do not have the capacity to manage a large outbreak, health experts and government officials have told IndiaSpend.
“We should not declare ourselves COVID-free…Instead, we should say, COVID not detected,” said Sedevi Angami, director of the Christian Institute of Health Sciences and Research in Dimapur, Nagaland.
After a lockdown of about 40 days, the government divided the country’s districts into red, orange and green, with red districts continuing to have stringent lockdowns, with limited permission for social and business activities, and green zones opening up with social distancing and other precautions.
In the northeastern region, only seven districts are orange (four in Assam, two in Tripura, one in Meghalaya), one district is red (in Tripura) and the rest are green. Assam, Tripura, Arunachal Pradesh, Meghalaya, Mizoram, Manipur and Nagaland combined have 101 COVID-19 cases.
These states have conducted 22,202 tests, almost 1.9% of the country’s total. Yet, at roughly 494 tests per million (as of May 4, 2020), this is about half the Indian average--851 per million (1.19 million tests in all).
Should there be an outbreak, there would be a lack of testing facilities, skilled staff to manage it, as well as inadequate infrastructure such as hospitals, isolation beds and ventilators, our reporting shows.
Lack of testing facilities
On March 24, 2020, when Prime Minister Narendra Modi announced the national lockdown, there were nine government COVID-19 testing labs--five in Assam, one in Meghalaya, one in Tripura and two in Manipur. Samples from Mizoram, Nagaland, Meghalaya and Arunachal Pradesh would be sent either to Dibrugarh, Barpeta or Guwahati in Assam.
Since then, one more lab each has been approved in Mizoram and Arunachal Pradesh and two more have been approved in Assam. No private laboratories in the region were testing samples, as of May 4, 2020 although they are being encouraged to set up facilities in Assam, according to this May 3, 2020 article in The Indian Express.
The closest testing centre was 370 km away from Dibang Valley in Arunachal Pradesh in Assam’s Dibrugarh district, said officials in a National Preparedness Survey, published on April 1, 2020.
On May 1, 2020, the Tomo Riba Institute of Health and Medical Sciences (TRIMS) in Naharlagun, Arunachal Pradesh, a sampling centre, was converted into a testing centre. No samples had been tested there, as of May 4, 2020, M. Lego, director of health services in Arunachal Pradesh, told IndiaSpend.
Until the first case in Meghalaya, on April 13, 2020, the testing laboratory in the North Eastern Indira Gandhi Regional Institute of Health and Medical Sciences (NEIGRIHMS) could only test 50 samples per day. The rest were sent to a medical college and hospital in Barpeta, Assam. “The capacity in Meghalaya has now increased to 99 samples per day,” Matsiewdor War Nongbri, the deputy commissioner of East Khasi Hills, told IndiaSpend.
Meghalaya also has a shortage of laboratory staff. On April 24, 2020, its National Health Mission announced vacancies for 10 laboratory assistants, 10 project associates and five medical microbiologists.
Tripura is an exception; the state has tested a high proportion of its population--5,162 per million. It has detected 40 new COVID-19 cases, as of May 5, 2020.
Tripura has an intensive surveillance strategy, where the state not only tested those coming from hotspots, but anyone who reported a cough or a cold for a prolonged period of time, said Sanjay Kumar Rakesh, the Additional Chief Secretary for Health and Family Welfare in Tripura.
“We realised that if our detection gets delayed and we don’t capture, then it would spread. Before the symptoms matured we wanted to detect it,” he said. The strategy “partly” emanates from the South Korean model but due to resource constraints, Rakesh said, they could not test as intensively. Tripura also randomly tests those who come from other states.
Tripura is conducting 300 tests a day but has a capacity of 600-900 a day, Rakesh said. “We have enough kits in stock in case there’s an outbreak,” he added.
Tripura was declared ‘COVID-free’ on April 25, 2020, but 27 people--including 25 BSF personnel and their close contacts--tested positive on May 1, 3 and 4 in Dhalai district, which was declared a red zone. On May 4, 13 more tested positive.
Community transmission
Although many of the positive cases (33 in Assam, one in Manipur and one in Arunachal Pradesh) in the northeast were traced back to those who attended the Tablighi Markaz, a religious gathering, in Delhi, the government has been unable to trace the source of several cases, such as four in Assam’s Bongaigaon district and one in Guwahati. This has created a worry about asymptomatic carriers and community transmission.
The four cases, all from different areas, were detected during the first random sampling of 40 people who had flu-like symptoms, said Ratna Basumatary, the then joint director of the Bongaigaon District Health Service. One of them is a vegetable vendor, two are health department officials and one is a railway department official, Basumatary said. “They were symptomatic but had no clear-cut contact history, which indicates there could be community spread,” he told IndiaSpend.
In one case, the patient’s son had travelled to another state and had been in quarantine for 14 days. He tested negative but his mother tested positive after 30-40 days, Basamutary said.
Since March 15, 2020, the Indian Council of Medical Research (ICMR) has been checking samples of Severe Acute Respiratory Illness (SARI) patients at random to test for community transmission but this began in Assam only by April 15, 2020, said Lakshamanan S., the state director of the National Health Mission.
The person in Guwahati, Lakshmanan said, was not a case of community transmission.“We had checked more than 100 persons (through contact tracing) and none of them turned out to be positive. If this was community transmission, then after one month of the first detection, we would have had 50-100 cases but that did not happen,” he explained. It is possible that the patient has not given the right history or came into contact with someone who has yet not been tested, he added.
As many as 82% of the COVID-19 cases in Assam that were linked to the markaz (cultural gathering) were asymptomatic, said Assam’s Health Minister Himanta Biswa Sarma, at a press conference on April 18, 2020. About 11% reported a cough and 7% had sore throat, breathing difficulties and diarrhoea, he said. Even though Assam has the most cases in the region, and many were asymptomatic, the state has among the lowest testing rates in the country with 425 tests per million population. About 0.34% of samples tested in Assam have been positive, below the national average of 3.8%, data show.
As of May 4, 2020, only the Meghalaya state COVID-19 portal was tracking data on the range of coronavirus-related symptoms reported on a daily basis.
Meghalaya alone providing symptoms data
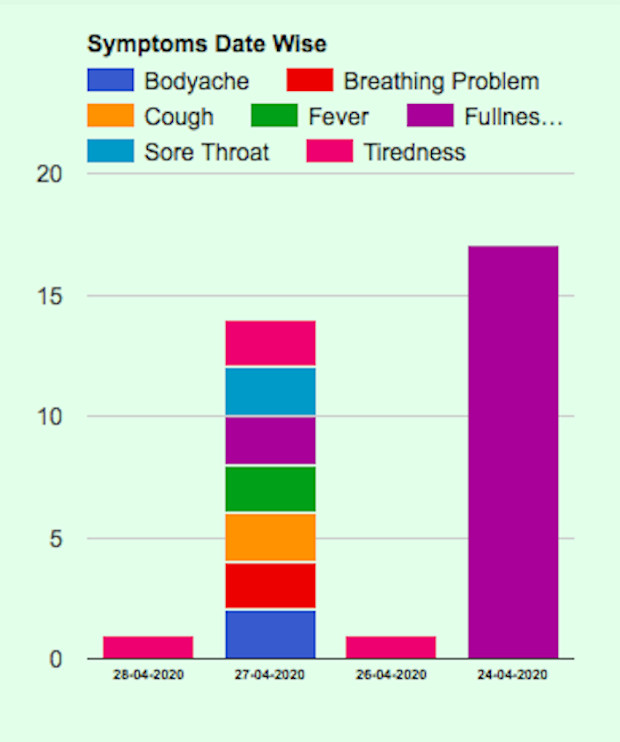
Source: Meghalaya State Covid-19 portal
Assam should be testing all patients with SARI, health experts and doctors told IndiaSpend.
The current ICMR testing strategy is sufficient but the government should make data public on the number of patients with SARI that have reported at government hospitals, along with details on how many have tested positive or negative, said Roshine Mary Koshy, a physician at Makunda Christian Leprosy and General Hospital in Karimganj, Assam. “This way we’ll know that the surveillance mechanisms are actually being implemented on the ground.”
Rapid testing
On April 23, 2020, with 9,600 rapid antibody test kits and approval from the central government, Assam started random testing in three containment zones--Spanish Garden and Athgaon Kabaristan in Guwahati and Lahorighat in Morigaon.
For surveillance of COVID-19 in the population, the government used antibody tests on 91 people, all of whom showed no signs of the virus, said Lakshmanan. For 25 of these samples, the government also did a reverse transcription-polymerase chain reaction (RT-PCR) test, which is the only test approved in India to detect COVID-19. All samples were negative, Lakshmanan said.
On April 27, 2020, the ICMR asked all states to stop using antibody testing kits, produced by the Chinese companies, Guangzhou Wondfo Biotech and Zhuhai Livzon Diagnostics, after complaints that the kits were faulty. However, the Mizoram COVID-19 tracker shows that the state acquired 1,085 rapid antibody tests of India after May 2.
Testing should be prioritised in the red zone (areas that have a high caseload, and contribute 80% of the state’s cases), to test for asymptomatic carriers and herd immunity, said Umesh Chandra Sarma, an epidemiologist and former director of medical education of Assam.
Herd immunity comes when a large chunk of the population is exposed to the virus but is able to fight and recover from it by developing antibodies against the disease. Herd immunity may not be effective as no evidence currently supports the theory in case of COVID-19 and there is a lack of knowledge on how long immunity lasts and the risk of re-infection.
Ill-equipped healthcare system in many districts
When the first COVID-19 patient tested positive on April 1, 2020, in Medo, Arunachal Pradesh, he was shifted to Lohit district hospital in Tezu. “We put him in an isolation ward, where he was administered with vitamin supplements, regular food, tea, warm water gargling and most importantly, counselling,” Sajinglu Chai Pul, the district medical officer, told IndiaSpend, clarifying that the patient was not administered hydroxychloroquine (HCQ), an experimental treatment for COVID-19 being used by many doctors in India and the world.
However, she added, if his symptoms would have progressed from mild to moderate (pneumonia), then he would have been shifted to either TRIMS (360 km away) in Arunachal Pradesh or Assam Medical College in Dibrugarh (176 km away).
TRIMS in Naharlagun and a general hospital in Pasighat are the only dedicated COVID-19 treatment hospitals in Arunachal Pradesh, the biggest northeastern state that spans over 83,743 sq km.
Healthcare infrastructure shortages have always been a chronic challenge in the region, said Priscilla C. Ngaihte, a public health specialist at the New Delhi-based Public Health Foundation of India, “Poor people tend to suffer for the lack of access to affordable healthcare because they can't travel and even if they get to the hospital, can't afford the treatment.”
Many hospitals do not have infrastructure such as CT scans, blood banks, oxygen, respiratory assist devices, monitors, personal protective equipment (PPE) and trained personnel, she said, commenting on the region’s preparedness in the event of a COVID-19 onslaught. She said that northeastern states should urgently prepare for an outbreak as the monsoon will soon make it difficult to move equipment, such as oxygen cylinders, by road.
Assam is one of three states in India with a severe shortage of healthcare infrastructure, according to a report in The Indian Express on April 27, 2020. Assam has 17 districts with zero ventilators--two of which are orange zones, according to the most recent classification of districts. Two of these districts, Morigaon and Dhubri, were red zones until May 1, 2020.
Dhubri, Golaghat and Nalbari had fewer than 100 isolation beds and there were no ICU (intensive care unit) beds in Dhubri, Morigaon and Nalbari, the report said.
In Assam’s Dima Hasao, district officials had said on April 1, 2020, that there was no ICU or ventilator in government hospitals, and no private nursing home in the entire district, as per a government survey on COVID-19 preparedness. Health Minister Himanta Biswa Sarma did not respond to our questions regarding whether the situation had improved in the past five weeks. “As far as I know, the Centre has always communicated that Assam is well placed with COVID-19 preparation,” Sarma said, responding to a question on this report, at a press conference on April 29, 2020.
“We can deploy as many ventilators on a war footing but these things will not help if the manpower is not available to handle it,” Sarma, the retired epidemiologist, told IndiaSpend, adding that the shortage was more of skilled human resources. On April 29, 2020, Sarma was appointed to an advisory committee on the utilisation of the Rs 107 crore deposited in Assam Arogya Nidhi (Assam Health Fund), the state fund to fight COVID-19.
There are similar issues in Arunachal Pradesh. There are nine ventilators in TRIMS and at least one ventilator in every district and zonal hospital in Arunachal Pradesh, said Lego, director of health services in Arunachal Pradesh. “But we don’t have as many anaesthesiologists. There’s a shortage of both man and machine,” he said.
“Even though ours is a general hospital, we did not have the facilities to treat the patient if he started showing aggravating symptoms,” said Pul, who treated the lone COVID-19 patient in Arunachal Pradesh. “Now, we’ve just got one ventilator but the installation is not complete.”
Nagaland has “half a doctor for every 1,000 persons”, with 28 doctors’ posts vacant in the Health and Family Welfare department and 27 doctors on leave, according to an article in the Morung Express, a local daily, on April 17, 2020. Since then, several retired health professionals, including doctors, nurses, and medical students have volunteered to help, the Morung Express reported on April 21, 2020.
Neither Health Secretary Kesonyu Yhome nor Chief Secretary Temjen Toy were available for comment, despite several calls and messages by IndiaSpend, on the number of doctors in Nagaland.
Nagaland’s first COVID-19 case on April 13, 2020 is being treated at Guwahati Medical College and Hospital (GMCH). This patient is not counted as a case in Nagaland because there is no testing facility there and the patient went to Assam for testing and treatment.
On April 15, 2020, upon visiting the Dimapur District hospital, the only COVID-19 dedicated hospital in Nagaland, former chief minister and opposition Naga People’s Front party leader TR Zeliang tweeted that there were only four ICU beds and ventilators available at the hospital. Until April 13, 2020, the hospital was unequipped to admit COVID-19 patients, reported the Nagaland Post, a local daily, on April 13, 2020.
Lack of personal protective equipment
Most northeastern states have a shortage of PPEs. Arunachal Pradesh has 1,500 PPEs, Manipur has 2,138, Mizoram has 2,658, and Tripura 9,000, according to data as of May 4, 2020. Experts estimate that a small hospital would require about 6,000 PPEs a month.
On April 15, 2020, nurses at the Dimapur District Hospital in Nagaland complained about faulty PPE suits saying that they “will not assist or attend any COVID-19 suspected cases without proper PPE”, according to their letter to the medical superintendent of the hospital. Dimapur district has 22,724 PPE suits, according to the Nagaland COVID-19 dashboard, the only state with a detailed live tracker on healthcare infrastructure.

A letter by nurses to the medical superintendent of Dimapur hospital, Nagaland
Returning migrants, porous borders
At the very least, one million migrants from the northeast region are living in other Indian cities. The most are from Assam (659,694), followed by Tripura (85,862), Manipur (75,751), Meghalaya (70,268), Nagaland (45,734), Arunachal Pradesh (37,368) and Mizoram (30,365), according to data from Census 2011, compiled by India Migration Now, a Mumbai-based research and advocacy organisation.
Since May 1, 2020, special trains set off from Kerala, ferrying migrants living in 20,000 relief camps all across the state. These migrants belong to West Bengal, Jharkhand, Uttar Pradesh, Orissa and Assam.
The borders of all northeastern states, other than Sikkim which has had no COVID-19 cases, have also been opened up for migrants. The returnees to Assam will be screened at inter-state borders for COVID-19 symptoms, and quarantined at home or in a facility for 14 days, the government has said. Only those showing symptoms are to be tested, as per the ICMR guidelines.
This will bring a fresh set of challenges for the region, particularly the repatriation of stranded people from major cities, particularly the hotspots, said Ngaihte, the public health expert. The “vulnerability of the northeast also lies in the porous border with neighbouring countries.,” she added, “Hence, containment of the virus will also be dependent on how our neighbours perform.” On different sides, the eight states in the region share long borders with Bhutan, Bangladesh, Myanmar and China. The region, experts said, should prepare for the worst.
Update: A previous version of this article erroneously said that the northeastern region had conducted 20% of all tests in India. The correct datum is 1.9%.Assam has one red district. At present, there are four orange districts in Assam and no red districts. While Bongaigaon was classified as a red district when the new four cases were reported (bringing the total to 5), it was later classified into orange district.
(Sitlhou is an independent journalist based out of Guwahati, Assam, covering the northeast region for national and international publications. She tweets at @makesyoucakes.)
We welcome feedback. Please write to respond@indiaspend.org. We reserve the right to edit responses for language and grammar.


