‘Not All COVID-19 Patients Need Antivirals. New Drugs For Restricted Use At Physicians’ Discretion’
Mumbai: The number of novel coronavirus infections continues to rise across the country, with some cities and parts of states considering going back into lockdown. The city of Chennai, for instance, has already gone into a second lockdown in anticipation of a higher number of cases and preparing itself for possible pressure on the health and medical systems.
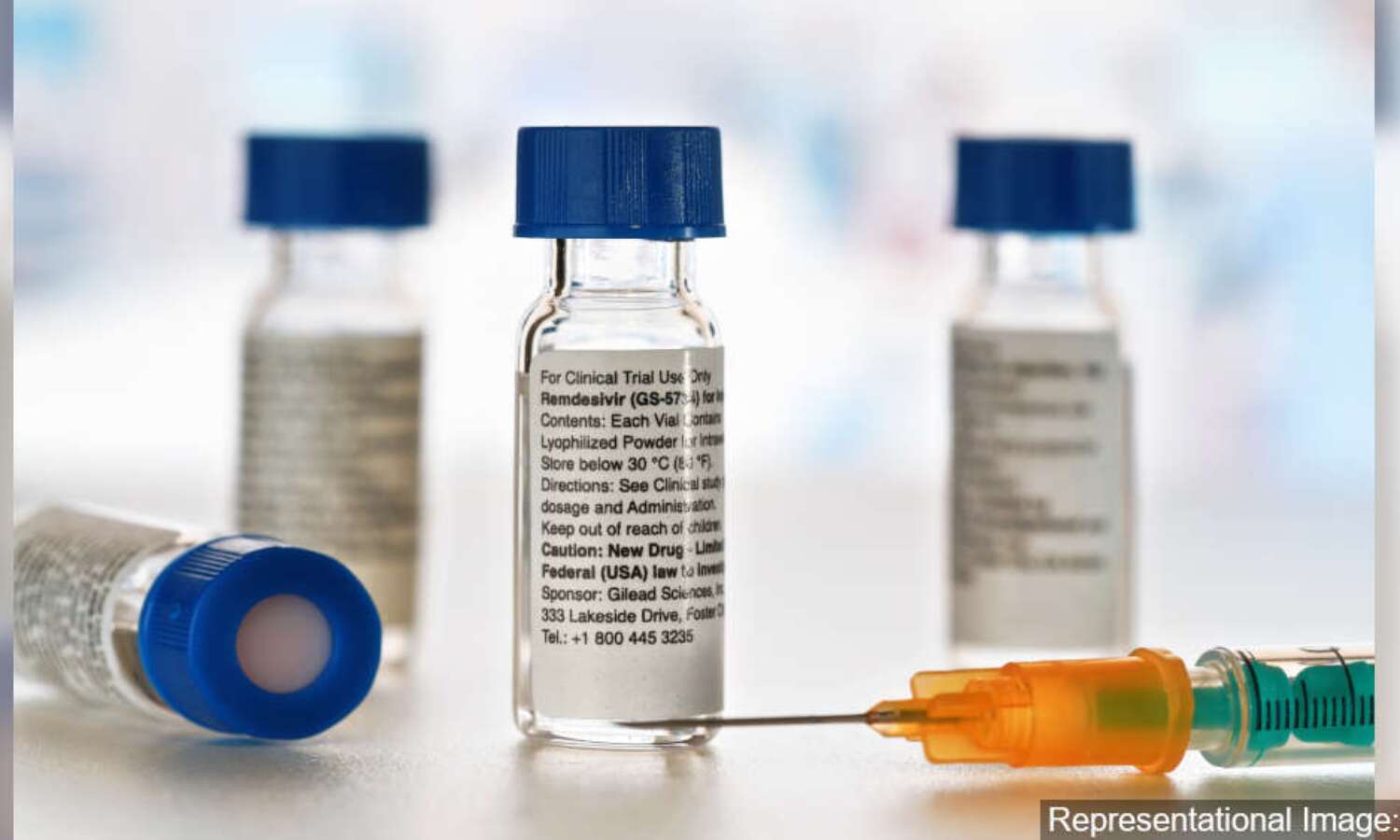
The good news, however, is that some marketing authorisations for drugs to treat COVID-19 have come through. Cipla Ltd and Hetero Drugs have got authorisations for antiviral remdesivir for restricted emergency use, and Glenmark Pharmaceuticals, a Mumbai company, has got an approval for manufacture and marketing antiviral favipiravir.
These medicines are likely to be available in the hands of medical professionals who are fighting COVID-19. How do these medicines work? What do we know of them today as opposed to what we knew of them earlier and what they were used for? And how are they likely to help the treatment of COVID-19 patients? We speak with Rommel Tickoo, associate director, internal medicine, at Max Healthcare, New Delhi.
Edited excerpts:
Remdesivir and favipiravir are now--or likely to be soon--in your hands formally. What does this mean?
As of now, we do not have any approved treatment for COVID-19. These drugs also, as you said, are meant only for emergency use, as in other countries like the US.
The DCGI [Drug Controller General of India] has approved favipiravir for restricted emergency use. It is actually a repurposed drug--it was earlier used to treat Influenza in Japan for many years, and then for post-exposure, prophylaxis and treatment of the Ebola virus. It is not a new drug. There are a lot of studies going on; more than 30 trials are going on in India, the UK, China, and Japan. We do not have enough data on it right now. Whatever data we have are very small, which are from these small studies done in these countries. It is mostly used in China, Japan, Russia and UAE. We cannot really go by these data; we need more evidence from large-scale, randomised controlled trials, which are happening right now. But it is going to take a while before we have the definite data and conclusion of these trials. Only then, we can seriously talk about the efficacy and safety of this drug.
But, the interim reports of, I think, the Glenmark trial--they are in phase 3 clinical trials--probably seem to be encouraging. That is why they have been given a go-ahead for marketing and manufacturing of the drug. Apart from that, there is not enough evidence as of now.
The catch here is that the mechanism of action of this drug is against the RNA polymerase, which is the enzyme meant for replication. So, it has to be given in the early stages of the disease. It is not meant for all COVID-19 positive patients. It is not meant for critical patients because by the time they are in that phase of the disease, they already have enough virus replication happening. For asymptomatic, mild young patients, there is no treatment required. So, you really have to choose your patient--mild to moderate ones. If it is proven to be efficacious and safe, then it might be a potential blockbuster drug in the sense that it can help prevent the progression to severity, and they might actually not get critical and need hospitalisation.
If we talk about remdesivir on the other hand, again, we do not have enough data on that [either]. In April, the National Institute of Allergy and Infectious Diseases in America came out with this interim report of the ongoing randomised, multi-centered trial. They said that it was not a totally knock-out drug, but it reduces the recovery time compared to a placebo from 15 days to 11 days. But, the effect on the mortality was not much: It [the mortality rate] was 11% [for those on placebo] and 8% [for those on remdesivir], which is not significant, statistically.
So, we need data on remdesivir also. There are a lot of trials going on--even in India, trials are going on; the Solidarity Trial is going on. But because we do not have any drug, and we cannot wait for the conclusion of these trials, and we have to save lives, I think that is the reason behind giving approval for emergency use.
But in these patients, lots of things are being used: We are using remdesivir, tocilizumab, we are using convalescent plasma, steroids. So, you really do not know what is helping them to get out of this. It is all anecdotal, based on the limited experience we have and the limited studies that are being done.
If we compare remdesivir with favipiravir, remdesivir is a drug that is intravenous, has to be given in a hospital setting, and is expensive. It is meant for critical cases, for people with moderate to severe disease, [the patients who] are on oxygen and in the ICU. Favipiravir is meant for mild to moderate cases, it is easy to administer. It is in tablet form, relatively inexpensive and has a good safety profile. So, both drugs have different sorts of patients to deal with. But the mechanism of the action is more or less the same; [they] work on the RNA polymerase and prevent viral replication. But you really have to choose your patient.
You have been treating patients, and I am sure you are having success at the mild to moderate stage, where you are saying that favipiravir plays a role. So, tell us about what is working at this point, and how could these potentially, if they work as advertised, contribute to your efforts.
Right now, we do not have any specific antiviral drug. We were using hydroxychloroquine, and in patients who have a cytokine storm going on, critical patients, we are using tocilizumab, which is not an antiviral drug. It is meant for the cytokine storm, where they have ARDS [acute respiratory distress syndrome], lung involvement and all the inflammatory changes happening. There, you use steroids and tocilizumab. Convalescent plasma is being used in moderate to severe cases, where there is impending ventilation required, [when] patients are getting sicker.
So, there is no specific antiviral drug we are using at this point of time. The only antiviral drug that we were using was the anti-HIV drugs, but there is not enough evidence that it really helps. So, in that sense, these are the main two antiviral drugs in our armoury right now. We will have to see how the experience goes. But whatever limited data are with us, it seems to be promising.
The last time we spoke, things were in much better control. But today many of the hospitals are overwhelmed, to put it mildly, and things are quite different. How are you seeing it?
Well, it was expected anyway. I think the last time we spoke, we were in the lockdown, so obviously the cases were fewer. But once the economy opened up, the offices started, the public transport started, the numbers were bound to go up. And there has been a spike, especially June onwards.
But we have to deal with it, we have to ramp up the healthcare infrastructure, keep adding more beds, and do more testing. We cannot just go by the numbers now. We are beyond numbers. They were anyway expected to go up, and we cannot focus on the numbers. We have to focus on saving lives now.
Nobody should die of COVID-19 and people should not run from one hospital to the other just because they are not getting a bed. That is going to be our focus. There has to be more transparency regarding the availability of beds. There have to be more beds available, and each hospital should have a help desk where somebody can guide them. If you land up in a hospital and there is no bed, [or] it is not a COVID-specific hospital, it does not mean that you have to run all over the city. There has to be some way of handling you, sending you in an ambulance to a specific COVID facility.
And [we have to] keep adding ICU beds, and hospital beds so that we have more oxygen beds available, because right now the focus is on saving the old and the vulnerable. They are the ones who are getting into trouble, and in whom the mortality is more. The younger ones, even if we get it, we have to isolate ourselves, take supportive treatment; we do not even need any specific treatment. So, the focus should be on ramping up the infrastructure, adding beds, saving the elderly and the vulnerable and saving more lives. And people should follow the norms and the protocols--wear a mask properly, maintain social distancing, hand washing. They have to be really particular about these things. They are not doing it well.
These two medicines--will patients ask for them? Or are doctors likely to administer them on their own? Will there be consent required?
Definitely, for restricted emergency use, you need to take consent. And as I said earlier, it cannot be given to everybody. You have to choose your patient who has the indication for this drug. As I said, remdesivir is more for the sick patients, the ones who are on oxygen or in the ICU; on the other hand, favipiravir is for mild-to-moderate cases and the decision lies with the physician. He will decide who needs which kind of treatment. Not everyone needs antiviral treatment, so we have to go with the analysis of the physician.
Do you feel now, even though the number of cases are rising, that your community is in better control of this disease, or are we roughly where we were two months ago?
The cases have gone up. So, we are dealing with more and more numbers and we are dealing with it because we have been adding beds, and hospitals. Earlier, there were very few private hospitals [treating COVID patients]. Now, there are more hospitals. Earlier, there was a lesser number of beds, [now, we are] ramping up the beds also.
So, we are dealing with it till now, but the only issue will be [when] more and more numbers are added and the cases go beyond the roof, then will we be able to handle it? Do we have enough manpower? Will we be able to ramp up the infrastructure more and more? That is going to be a challenge. Till now, we are managing; it is difficult, but we are managing. But time will tell us how it will unfold in the next few days.
We welcome feedback. Please write to respond@indiaspend.org. We reserve the right to edit responses for language and grammar.


