In A Mumbai Slum, Children Become Healthier, As Their Parents Learn To Tackle Malnutrition

Mumbai: “I think I perhaps knew how to hold a baby and play with one before I had my own, but not really anything else. I didn’t know what to expect when I got pregnant. Growing up, talking about diet and the best types of food isn’t really anything I remember,” recounted Sumita Anil Dhumale, 23, a mother of two.
Like many mothers with little education, who marry young and move far from home, Sumita had to fend for herself in an unfamiliar city with her first child, taking advice from her mother-in-law on feeding and hygiene practices. When it came to her second child, however, a local anganwadi (government-run child care centre) worker made sure she delivered at government-run Sion Hospital in central Mumbai and that the baby was taken in regularly for weighing and check-up sessions to monitor his development.
“I’ve learnt now to not make the same mistakes I used to,” Sumita told IndiaSpend on a recent August morning. “Earlier, I used to mix gripe water [a solution known to contain alcohol and other non-natural ingredients] in his milk to keep him quiet while I went to work. When I started visiting the anganwadi, I learnt this could damage the brain and affect his growth so I’ve stopped now.”

Sumita, 23, with three-month-old son, Rajiv, in the Mumbai slum of Dharavi. “I think I perhaps knew how to hold a baby and play with one before I had my own, but not really anything else. I didn’t know what to expect when I got pregnant,” Sumita recounted.
Outside the dimly lit single-room home that Sumita shares with her husband and two children, barefoot kids ran along narrow planks covering open drains. Fumes emanated from gas stoves on which lunch was being cooked in the cramped houses piled on top of each other.
Sumita is a resident of Palwadi, a low-income area in Dharavi, Asia’s third largest slum by population. Bandra-Kurla-Complex (BKC), Mumbai’s newest business district filled with shiny glass-front buildings and restaurants serving global cuisine, may be a 10-minute drive away but is a world removed. At Dharavi, sanitation and civic amenities are sparse, and the environment so polluted that residents are highly vulnerable to illness and disease.
The Society for Nutrition, Education and Health Action (SNEHA), a local NGO, has worked across 10 beats in Dharavi for five years, and its efforts have reduced wasting among children up to three years of age by 23% and produced a 109% increase in the services received by children in the area through the Integrated Child Development Services Scheme (ICDS), a government programme covering health, food and primary education, according to data recorded by SNEHA’s field staff.
Why malnutrition must be eradicated
Aahar--which means ‘diet’ in Hindi--is Asia’s largest urban malnutrition programme. Established in 2011, it aims to do reduce the prevalence of child malnutrition by increasing awareness of its risk factors and supporting the work of local anganwadis, which are run under ICDS.
Nearly 20% of children under five in India are wasted (have low weight for their height) and 7% severely wasted, according to data from the National Family Health Survey of 2015-16. This is up marginally from 19.8% and 6.4%, respectively, a decade ago, showing little improvement in a key indicator for child development.
Poor nutrition and subsequently illness in the first two years can cause lifelong physical and cognitive damage that is largely irreversible, affecting academic ability and adult health. This ultimately impacts negatively on a country’s economic output. Reducing nutrition deficiency amongst children under three years of age could increase the number of graduates in the country by 11% (3.17 million) and prevent a loss of 0.8-2.5% of GDP (equivalent to $15-46 billion).
Such failures in early-life nutrition are why Armida Fernandez founded SNEHA in 1999. After a decade of experience working at Sion hospital, she grew tired of seeing children slip back into malnutrition as soon as they were discharged and returned to the slums. She realised that community intervention was imperative.
“Malnutrition is not just a rural problem,” Anagha Waingankar, associate programme director at SNEHA, told IndiaSpend. “There is a lack of support networks [in urban areas], whereas in the villages pregnant mothers will have support from the extended family.”
“In rural areas, malnutrition may be about access to food, but here the profiles you see are different. Often the mother works as domestic help, the dad is in the factory and children are just left with siblings to manage their own eating,” Waingankar said.
SNEHA’s baseline data from a 2016 survey of children up to three years of age in Dharavi show 18% were wasted and 24% stunted (short height for age).
Using a model based on the World Health Organization’s Community-based Management of Acute Malnutrition (CMAM) principles, SNEHA tackles gaps in nutrition understanding amongst the community to improve its overall health status.
Often dealing with mothers who fear the stigma of speaking openly about their child’s illness, recent migrants with no knowledge of the area and its public health services, plus an under-resourced network of anganwadis, SNEHA trains men and women from the communities it serves to better understand and help address these issues.
Many who begin as community volunteers working in their spare time to educate neighbours on nutrition best practice and encourage the use of local health facilities, go on to become full-time paid ‘community organisers’ (COs). Leveraging years of valuable on-the-ground experience, they train and support sevikas (anganwadi workers) to improve their understanding of nutritional science and accurately record data to monitor each child’s progress.
“Before I joined SNEHA even my own daughter was malnourished, I made mistakes,” Lakshmi, 37, a CO and Dharavi resident, told IndiaSpend one rainy August morning at the Aahar programme office near Matunga Labour Camp, a mixed-use area of low-grade housing and light industry. “She used to fall sick every month up till the age of five, but now she is doing much better. I’ve learnt to practice good dietary diversity and hygiene at home.”
Plugging awareness gaps
SNEHA taps into the community volunteers’ knowledge of who may be pregnant, has recently moved to the area or is struggling to feed a newborn, and shares this information with anganwadi workers. Subsequently, anganwadi workers are able to improve their involvement in the community, develop close relationships and talk sensitively about the problems associated with poor hygiene and nutrition.
That means women like Farida Shakir, a 30-year-old resident of Dharavi, are a crucial component of a model which aims to drive behaviour change and increase awareness of health best practices.
“The community organiser and sevika kept visiting my area and I heard them talk a lot about immunisation and carry out check ups on the local children,” said Shakir. “Since my kids are all grown up I liked the idea of being with little ones again and felt I’d be good at this work and decided to volunteer. People used to think they had enough knowledge of their own to get by but now they are ready to listen.”
Holding an infant on each hip, neighbour Kushanna entered Farida’s single-room residence and began praising her work. “Farida and I really have a mother-in-law and daughter type relationship. She gives good advice, like if I need to take one of the children to the hospital,” Kushanna said. “When I was pregnant she told me what to eat and how to look after myself, I’m now more aware about good practices. I know that the most important thing is to keep the house clean and give food on time.”
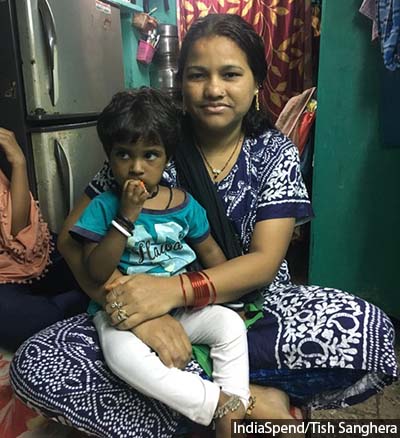
Farida Shakir, 30, a SNEHA community volunteer in her home in Dharavi
But it often takes time and relentless engagement to reach a stage where mothers are as receptive as Kushanna to listening to and heeding well-intentioned advice.
For instance, it can be difficult for families to hear that a child is malnourished and its significance does not always register immediately. Parents are used to comparing the child’s body to other family members’, thinking they will catch up and that for the moment everything is normal.
By 2015, the end of the first phase , Aahar had reached an estimated 31,000 children and 6,000 pregnant women across 10 beats in Dharavi. However, these figures hide the challenges of working in this area and the complexities often involved in each case.
Often, a subtle negotiation of family dynamics and individual circumstances is needed to effectively discuss the sensitive issue of a child’s health with a mother, Bharti, a 41-year-old resident of Wadala and a SNEHA CO, told IndiaSpend. She described a familiar scenario of a woman who had recently arrived from rural Uttar Pradesh with a six-month-old baby: “She was completely blank about nutrition paths and her family didn’t let her leave the house, so it was difficult for her to get to know the area. It was lucky the sevika and I found her because her child was sick and their general hygiene not in a good condition.”
“Since she was reluctant to listen to us we came back at 4 p.m. when her husband was back from selling vegetables. We managed to persuade him to bring the child to the anganwadi and get him immunised--they thought since they as parents were not immunised, the child would be fine,” Bharti said, “Now the child visits the anganwadi every month and is doing well.”
High inter-slum and intra-slum migration is a major reason why some children slip through the net of local health services. With up to 30% of the population changing every month, it can be difficult for sevikas to find those in need, SNEHA has observed. Inevitably, it is the youngest children under three who suffer the most as their feeding and environment changes; even healthy children can fall ill.
To keep revisiting households and reinforcing the health messaging they’ve been taught appears to be working. SNEHA’s Aahar army are now a recognisable force for good in the community, and barriers to their acceptance have come down. Mothers in the area are better informed.
“The first time we used to knock, they closed their door without waiting to see what we are asking or why we are here,” said Lakshmi. “One mother told me ‘no, we don’t go to the anganwadi for weighing sessions since we don’t want our child to catch nazar [the evil eye]’, but now people recognise our blue SNEHA coats and they are ready to listen and participate. Things are changing.”
Supporting ICDS workers
Difficult conditions, a lack of training and burdensome paperwork mean the 1.34 million-strong network of anganwadis operating nationally is heavily strained.
Just 29% of these basic family health centres were able to deliver all six of the services mandated by the ICDS (which include immunisation, supplementary nutrition and medical referrals), according to this 2013-14 report by the Ministry of Women and Child Development. Nearly 68% had no electricity connection, 57% no toilet facility and 65% no water facilities on the premises.
In 2016, SNEHA signed an agreement with the ICDS and the Municipal Corporation of Greater Mumbai (MCGM) to form the Mumbai Child Health and Nutrition Committee (MCHNC).
While the first phase of the Aahar programme saw its staff working directly alongside anganwadi workers, the post-2016 phase has focused on supporting ICDS staff to deliver their six key services, as well as to coordinate on data and resource deployment.
Low and often irregular pay, coupled with a lack of guidance and feedback from managers, mean many anganwadi staff can feel a lack of motivation to engage with their work. Many do not receive adequate skills-based training or mentoring, and SNEHA tries to fill this gap.
Each anganwadi is visited four times in a month by a SNEHA CO, who has five anganwadis under her care. Activities are planned out for the month, events organised and child health data recorded. A flashcard game that taught the nutritional content of food was being explained for use at a nutrition drive at the end of the week when IndiaSpend visited.
“I’ve learnt a lot of useful ‘tricks’ from the SNEHA COs. Their training has helped us deal with a lot of issues that we regularly face,” said Noorjahan Kamble, 44, an anganwadi worker in Palwadi, Dharavi. “Sometimes parents don’t want to hear our advice but they have taught me how to speak with authority and explain things differently in a way they can understand.”

Jamila Sheikh, 30, a SNEHA Community Organiser, and Noorjahan Kumble, 44, an anganwadi sevika.
The benefits of supporting health workers and mobilising local communities have been evident. Working with the most vulnerable communities only, Aahar’s second phase has reduced its coverage in Dharavi from 10 beats to three, following large improvement in the area. Its success means it has now expanded into two beats of Wadala, a neighbouring area with a similarly high prevalence of malnutrition.
Here, the challenges the programme faces are the same--low awareness about the importance of good nutrition among time-strapped parents labouring for a daily wage.
“I really hate leaving the kids alone at home, but there’s not much else I can do. I have to go to work in the daytime and then I come home around six,” said Sumita, who we met earlier. “I leave home-cooked food for them before I leave, but I don’t really know what they get up to during the day.”
Mothers like Sumita are now at least aware of the importance of good nutrition and making use of the available ICDS services, even if they are not always able to stay home with their children. As a rag-collector who uses the income to buy utensils which she can sell on the streets, her children being ill is not something Sumita can afford. She takes the health advice given to her seriously and her positive experience with the public health system is something she is now keen to share with others.
“There was a woman down the lane who I met a while back and she was five months pregnant. She was new to the area so I made sure she was visiting the anganwadi and learning about pregnancy care,” said Sumita, smiling at Noorjahan, her local sevika. “Just like I learnt from ma’am.”
(Sanghera is a writer and researcher with IndiaSpend.)
We welcome feedback. Please write to respond@indiaspend.org. We reserve the right to edit responses for language and grammar.


