Scare of the Scars: Acid Attacks and Skin Scarring
Acid causes severe damage as it eats away at the skin and muscle tissue layer by layer. We talk to an acid attack survivor and to doctors to understand how acid burns are treated and what could make the medical ordeal easier for them
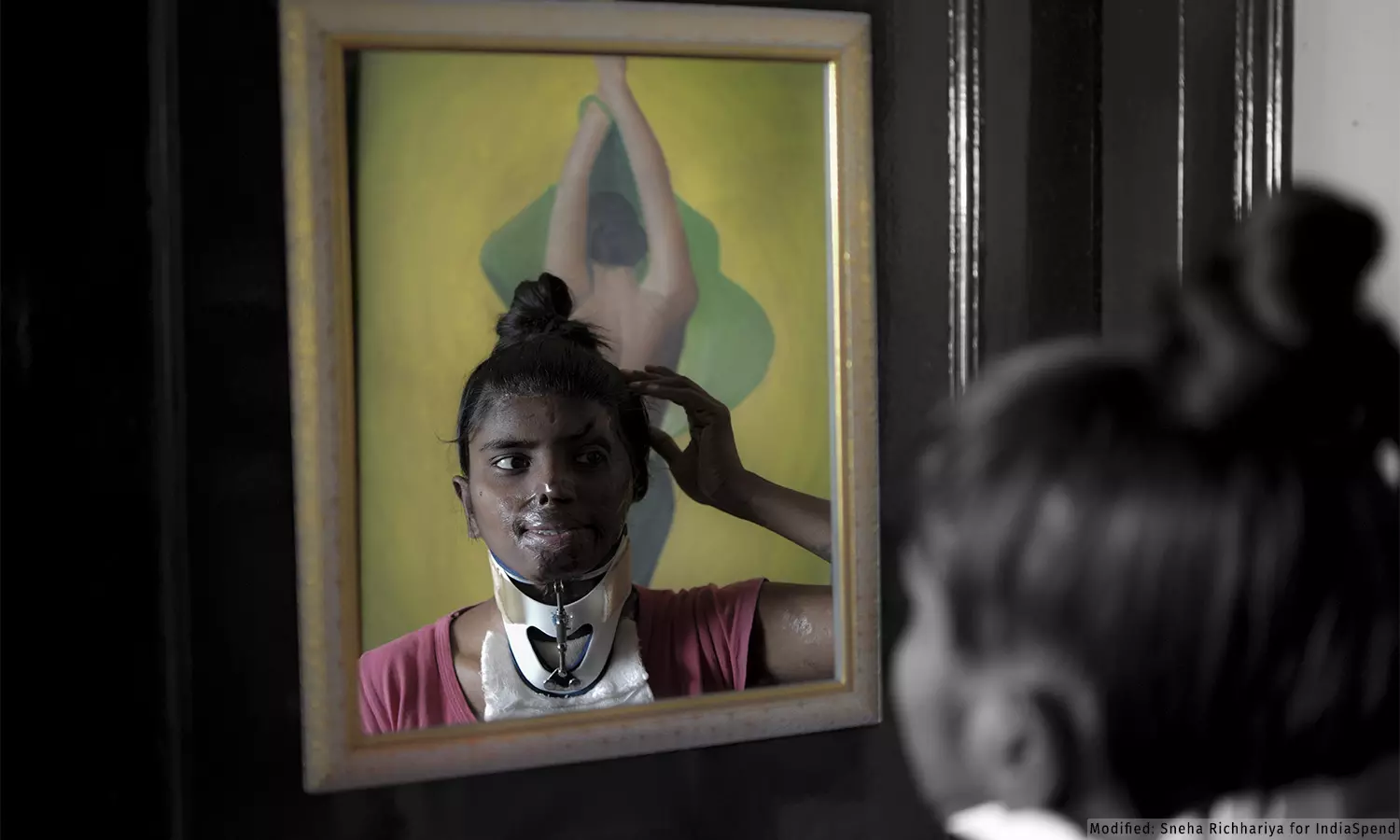
Seema was attacked with acid in 2016, leaving most of her skin severely burnt. Here, she looks into the mirror as she gets discharged from AIIMS, New Delhi after her skin grafting operation.
New Delhi: Seema, 24, is perched on a swing, peering at a borrowed mobile phone as she attends an online English class.
She notices me, turns the phone off and limps towards me. She has just returned from the All India Institute of Medical Sciences (AIIMS), Delhi, after spending over 10 days undergoing what is her 13th skin graft operation. At least, she thinks it is her 13th--there have been so many, she is losing count. This time, skin from her right leg was grafted onto the badly burnt area around her neck.
In 2016, Seema was just 18 and about to give the Grade XII board exams when she was attacked with acid. She recalls that she had left home early that morning--there was no toilet at home; the family members usually used a nearby field. “It was 6 am They came in a Scorpio. There were three people in the car; the one who attacked me was sitting in the back.”
“There was nobody around. I shouted out in fear and pain and ran straight towards my home. My skin started to shrink, and there was steam coming from it, just like you see in cooked rice,” she says. “I fell near the entrance, just as I saw my mother.”
Seema’s father is a farmer who also runs a small momo stall in Akbarpur Tehsil of Ambedkar Nagar district in Uttar Pradesh. The attack on her was “revenge” because her elder brother had refused to marry his friend’s relative.
The Ministry of Health and Family Welfare, in its 2021-22 annual report, stated that India records an estimated 7 million burn injuries per year and an estimated 140,000 deaths, making burns the second largest group of injuries. “Death and disability due to burn injury are preventable to a great extent,” the report says, “provided timely and appropriate treatment is provided by trained healthcare professionals.” Burns from acid are chemical burns, and harder to treat than thermal burns, doctors say.
According to data from the NCRB, crimes against women in India increased by 15.3% in 2021, and the rate of cases per 100,000 women population increased to 64.5 in 2021 from 56.5 in 2020. NCRB recorded 1,070 acid attacks against 1,115 victims in the five years from 2017 to 2021. Of these, 636 attacks were recorded against 656 women victims. In 2021, as per the latest available data, 176 acid attacks were reported, along with 73 “attempts to acid attack”. Of these, 102 attacks were recorded against 107 women.
“We do not have a separate record of chemical burns so far. All the data on acid attacks we have is from NCRB [National Crime Record Bureau],” said Manas Pratim Roy, the additional director general for non-communicable disease under the Directorate General of Health Services of the Ministry of Health and Family Welfare. RV Yadav, from the women safety division of the Ministry of Home Affairs did not provide information on recording of acid attack cases, police sensitisation or data on chemical burns over the phone and asked us to email. We had not received any response by the time of publishing and will update the story when we receive a response.
According to Acid Survivors Trust International (ASTI), a UK-based nonprofit with local partners in six countries including India, in almost 76% of cases, the attack is committed by a person who is known to the victim. Unlike Bangladesh, where most attacks occur in the home, attacks in India often occur in public places such as roads, schools and colleges.
Seema sits in her dark room as she takes a break from her daily routine
As in Seema’s case, open defecation is one of the major threats to the safety of women as it makes them vulnerable to violent crimes in secluded areas, mostly during night time and in the early hours of the day. One in three women in households without toilets reported facing sexual assault, according to the 2016 Rapid Survey on Gender Norms and Sanitation and Hygiene, and Implications, cited in the Economic Survey 2016-17. Further, 34% women from such rural households reported facing assault, as did 30% from urban households. A 2016 study found that women who defecate in the open were twice as likely to face violence as compared to women with a household toilet.
This is the second article in IndiaSpend’s ‘Acid Attack’ series, which dives into the systemic health issues that acid attack survivors face to regain their vision and reconstruct their skin, and also explores health systems response, policy interventions and medical accessibility for survivors. You can read the first part, on an acid attack survivor's journey to regain sight, here.
Stages of damage to the skin
Doctors explain that acid causes severe pain and damage as it eats away at the skin and muscle tissue, layer by layer. It gets through the two layers of the epidermis into the underlying fat and muscle, and occasionally all the way to the bone, which could cause the bone to disintegrate.
The severity of the damage is determined by the acid's strength and on how long it was in touch with the skin; the burning lasts until the acid has been completely removed with water. After an assault, a victim's epidermis frequently develops white patches within a few days. These areas eventually develop a darker hue. The underlying skin will appear raw, fleshy, red and inflamed, once the dark and damaged skin has fallen off.
“Initially, nobody could figure out what had happened,” Seema says. “My brother took me to the nearby district hospital on a bike as my skin kept emitting steam.” There, the attending doctor took two hours trying to clean the skin with saline solution before informing Seema’s family that they would not be able to treat her. They gave her a “cream” to apply, and suggested taking her to Lucknow.
When I met her in March 2023, she had just undergone her 13th skin graft. Pointing at her legs, she says, “There is no area on my legs from where skin has not been taken out. They have put it all on my face.”
The process of taking skin from one part of the body to replace damaged skin on another part is called skin grafting.
Seema shows her neck which was grafted on March 1, 2023
Understanding injuries to the human skin
Whenever there is a burn injury or a chemical injury, Shivangi Saha, a plastic and reconstructive surgeon and an assistant professor at the AIIMS, Delhi, who has operated on Seema, explains, “there are three different wounds according to the Jackson Zones of injury.” The innermost zone is the zone of coagulation. This undergoes energy damage and becomes dead. This is followed by an area which immediately surrounds it, which is called the zone of stasis. Here, if good first aid is given to the patient, then there is a chance that it can be salvaged. The third and outermost zone is the zone of hyperemia, which initially looks reddish, but this zone heals once the patient starts to recover.
“Depending on the depth of injury,” says Saha, “there can be a superficial injury, which involves only the superficial epidermis and dermis; there can be a deeper injury, which involves the deeper layers of the dermis and the subcutaneous tissue. And there can be a very deep burn which is also known as a third degree burn. The superficial burns can heal without surgery whereas deep burns and third degree burns always require surgery to heal.”
What survivors face with skin injuries
Seema combs her hair from front to back in an attempt to cover her bald scalp. “I don’t have hair on the top of my head,” she says. “So I have to do this.”
She is slowly coming to understand how the injuries have affected even things that she otherwise took for granted. The grafted skin, she says, does not sweat as it may not have oil glands--and the burns can also affect the skin’s ability to maintain body temperature.
Seema shows her hand [left], which was grafted years ago
“The function of skin in the body is also to maintain temperature. When burns happen, the skin is lost, the protective layer is lost. So the person may lose a lot of heat initially just after the burn injury, and it causes a condition called hypothermia,” explained Vijay Kumar, professor & head of the department of Plastic & Reconstructive Surgery at King George’s Medical University in Lucknow. He saw Seema when she was taken from Akbarpur to Lucknow for the first time in 2016.
Hypothermia is when the body dissipates more heat than it absorbs or creates, leaving the body unable to generate sufficient heat to maintain homeostasis, meaning the state of balance and proper bodily function. “When it's been a while after the burn injury, after three, four days, then to heal the body, the body cells start producing a lot of heat--it's called a hyper metabolic response to burn injury,” Kumar explains.
In this hyper metabolic response, the body will burn a lot of energy inside the body to make up for the heat that is being lost. This leads to increased body temperature. Severe burn injury is followed by a hypermetabolic response that persists up to 24 months after injury.
“We are looking forward to [medical] improvements in hair grafting because in a lot of these patients of acid attack, hair is lost and the eyebrows too,” Kumar says.
Seema suffered burns over almost 80% of her body in the attack, including her head, right ear, lips and nose. “I spent all my time locked in a room,” she says. “I did not see any visitors for long.”
“My body and face looked so bad that even my mother fainted seeing it. I did my dressing myself because nobody would want to touch these scars.”
In pictures clicked just after the attack, Seema’s lips look severely swollen and her nose shrunken. “I have had some 13 surgeries to get to what I look like now--but even this isn’t normal, you see?”
Treating acid burns on the human skin
The quality of recovery depends in large part on the first aid provided in the immediate aftermath of an attack. And the person who provides the first aid has to first protect himself or herself by wearing some kind of protective equipment, Saha said.
The second thing to do is provide first aid. Saha explains, “By first aid, I mean using water--and only water. It should be at normal temperature, ideally running water but absent that, use a bucket or any other vessel. You do not use very cold water because that can further aggravate the injury by causing spasm of the vessels surrounding the area.”
“And then for 20 minutes or till the pain is released, you keep on washing the affected area so that the acid agent is washed off from the body. One thing that is often ignored but very essential, is to isolate the acid burns from the rest of the body.”
I had first met Seema a year ago. Then, she was always on her own, mostly silent, never smiling. At this second meeting, though, after her latest round of surgery, she was more forthcoming as we sat in her darkened room. Shy and the youngest of several acid attack survivors who live together, she often spends time alone in her room. “I can never forget that four-hour drive from Akbarpur to Lucknow--the most dreadful four hours of my life.”
On reaching Lucknow Medical College around noon, she went through her first skin graft. “They took skin from my left leg.” Kumar, who operated on her then, says, “There are also procedures where skin is taken from a relative or an unrelated donor. It can even be taken from a dead body.”
Seema shows her right leg from where skin was taken for grafting on her neck
In such operations, a section of the epidermis and dermis from one part of the body--the donor site--is first completely separated from its blood supply, before being transplanted to another area of the body, the recipient site. Such operations are mainly done when there are raw areas, with no skin, over the body.
“Other procedures that can be done for such victims are different kinds of reconstructions,” Kumar explains. These reconstructions can use a skin graft, they can use flaps [tissue attached to blood supply], they can use different types of releasing and reshaping surgeries. “Like, if you have to make the eyelid, you do a release surgery [which releases the muscles, skin and nearby tissues contracted because of the acid] and then you put skin graft over the eyelids to make new eyelids.”
In some cases of acid attack where the neck gets stuck to the chest--a disfiguring condition, called a contracture--skin grafts are done on the neck area after releasing the contraction.
Kumar says, “hair transplants can be done to create eyebrows, eyelids and eyelashes. Skin from the forehead can be used to create the nose. Skin from the scalp and rib cartilages from the chest can be taken to reconstruct the ear.”
Cosmetic surgery: rewards and risks
The surgery that was performed on Seema is a blend of cosmetic and reconstructive surgery. Technically, cosmetic surgery is only done after all the reconstructive surgical procedures are complete. “Once the disfigurement is reduced over time, the face becomes better and better,” Saha, the surgeon at AIIMS, explains.
Seema once asked her mother if she was looking for a boy for her to marry. “Who will marry you?” her mother said. Seema has a twin sister for whom the family is looking for a suitor.
Seema always carries old pictures of herself. She says she was fond of getting pictures clicked
“I have always seen my face and body changing,” she says. “The doctor said I can also get my nose and right ear corrected, but I am tired of it now.”
Seema is not sure if her initial surgeries have helped her much. “I had developed some infection,” she said. Kumar, who operated on her at KGMU in Lucknow, says that he doesn’t remember Seema’s particular case but some of the infections can be treated with antibiotics while others need surgeries.
On why despite 13 surgeries, Seema’s improvement is disproportionate, Kumar said, “With a lot of these procedures, it is not possible to get very good results in one stage. Such patients need multiple procedures over a prolonged period of time. And even after surgery, physiotherapy and rehabilitation is very important--if they don’t undergo physiotherapy and rehabilitation, they may again develop scarring.” Seema has not undergone physiotherapy or rehabilitation.
Health system response
On reaching Lucknow Medical College at noon on the day she was attacked, Seema recalls being told to wait. “We were asked to fill some forms.” From the emergency ward, a patient is generally transferred to the surgery room. “I was taken to the surgery room at 4 a.m. the next day, almost 14 hours after I reached the hospital. I stayed in the emergency room for the whole night.”
Most survivors of acid attacks that I have met tell similar stories of long waits in hospitals. These delays are a double whammy for the patients--the effects of the attack are bad enough if first aid and treatment is administered immediately; the longer the duration from attack to treatment, the more time the acid has to do damage and consequently, the more complicated the recovery process, doctors have told me.
Shahin Nooreyezdan, a plastic surgeon at Apollo Hospital in New Delhi, tells me that the function of a primary and a secondary healthcare setup, including district hospitals, is to provide first aid and refer these victims to a tertiary facility. “We usually encounter acid attack cases much later, when they’ve already lived with the wounds for years,” he says. “We are a private facility. Most of these patients cannot afford it, and so they are brought to us by NGOs.”
“Apart from the medical advancements in using a dead person’s skin for grafting and manufacturing artificial skin in the laboratory, we need more emphasis on bringing the treatment cost down by investing in further research and innovation,” Saha says.
“The treatment for acid attack survivors at all government and private hospitals is free and unavoidable, irrespective of the patient's ability to pay,” said Roy of the health ministry. "There are other provisions where the patients can get funds from the government.” Based on a Supreme Court judgement, the Ministry of Home Affairs had asked that no public or private hospital deny treatment to the victim of an acid attack. The government also provides compensation of ‘at least Rs 300,000’ from the Victim’s Compensation Fund and of Rs 100,000 from the Nirbhaya fund.
In January 2021, then Union health minister Harsh Vardhan inaugurated a 100-bed dedicated facility to treat patients suffering from burn injuries at the AIIMS Trauma Centre in Delhi. Until then, most burn patients were taken to Safdarjung, Ram Manohar Lohia or Lok Nayak hospitals.
The new facility has six operating rooms, 10 private isolation chambers, and 30 individual ICU cubicles. Additionally, it has areas set aside for the construction of facilities for skin banking, children's physiotherapy, hyperbaric oxygen treatment, and hydrotherapy for burns, among other things.
On March 1, 2023, at this new facility, Seema was operated on along with a group of four other acid attack survivors. “We operated them together because then a single caregiver can take care of all of them together,” Saha tells me.
Photo credit: Ritu Saini, a fellow acid attack survivor and Seema’s friend
After a week of her operation, Seema along with other survivors, was shifted to the AIIMS guest house. “We were supposed to stay longer there, but we came home because it wasn’t very comfortable,” Seema told me. When I saw her shortly after her return, she was unable to walk straight, because her legs were still feeling the effects of skin being removed to be grafted elsewhere.
Policy interventions
“AIIMS has been working on a lot of policies with the government, but few of them are in process,” Saha says. “And because there is some red tape around it and till the policies are actually published, I cannot disclose much.”
She says, however, that the government is trying to come up with a workable referral policy so that these patients can be easily referred to a tertiary hospital when they need appropriate care. “The government under the National Programme for Prevention and Management of Burn Injuries (NPPMBI) is trying to build the capacity and train a lot of medical persons including doctors, nurses and dressing assistants [for treating burns].” The NPPMBI is a pilot programme initiated in the year 2010 with a budget of Rs 29 crore.
In order to raise awareness about burn prevention and prompt treatment, the ministry launched this pilot project in three medical schools and six district hospitals in Haryana, Himachal Pradesh and Assam. In 2014, the pilot became a full-fledged programme, the National Programme for Prevention and Management of Trauma and Burn Injuries (NPPMTBI), with a plan to set up burn units in 67 state government medical colleges and 19 district hospitals during the 12th five-year plan (2012-2017). The scheme was then extended to March 2020.
For the 67 planned burn units, 47 medical colleges have been approved and 17 district hospitals identified for financial assistance.
The scheme was brought under the umbrella scheme-‘Tertiary care Programmes’ of the Ministry of Health & Family Welfare until 2020, to which both the central and the state governments contributed. Since 2019, the programme has been under the National Health Mission.
Commenting on the status of the programme, Roy, additional director in the health ministry said, “We identified centres from all over the country and proportionally shared funding between the central and the state governments. There were mainly three things--building infrastructure, procuring equipment and hiring/training manpower…Some of it has already been implemented. We are still procuring equipment but it has been delayed due to COVID-19 and other reasons.” He did not provide any data.
According to PRS Legislative Research, an independent policy research organisation, more than 65% Indians do not use government health facilities because they are too far, are inadequately staffed and offer poor services.
Private hospitals are not an option for many, given the expense. In the aftermath of her attack, she had spent eight full months in the hospital in Lucknow, which would have been impossible given the state of the family finances--she was able to get tertiary treatment only because of support from an NGO.
Recalling those traumatic first few months, Seema says that she saw herself for the first time in the mirrored side of a hospital lift. “There was dressing all over my body. I could see only one of my eyes.”
Seema wears her neck brace before she leaves for her class
As she gets ready to leave for her offline English tuition class, she tells me, “I don’t cover my face here in Delhi, but even today when I go home (to her village in Uttar Pradesh), I have to cover my face because my family wouldn’t like it.
“Here in Delhi, I am free,” she says as she picks her bag and leaves for her class.
(This article was supported by Health Systems Transformation Platform as a part of the HSTP–Health Journalism Fellowship 2022.)
We welcome feedback. Please write to respond@indiaspend.org. We reserve the right to edit responses for language and grammar.


