Among Muzaffarpur’s Children, 2 In 5 Are Underweight, 1 In 2 Too Short For Age
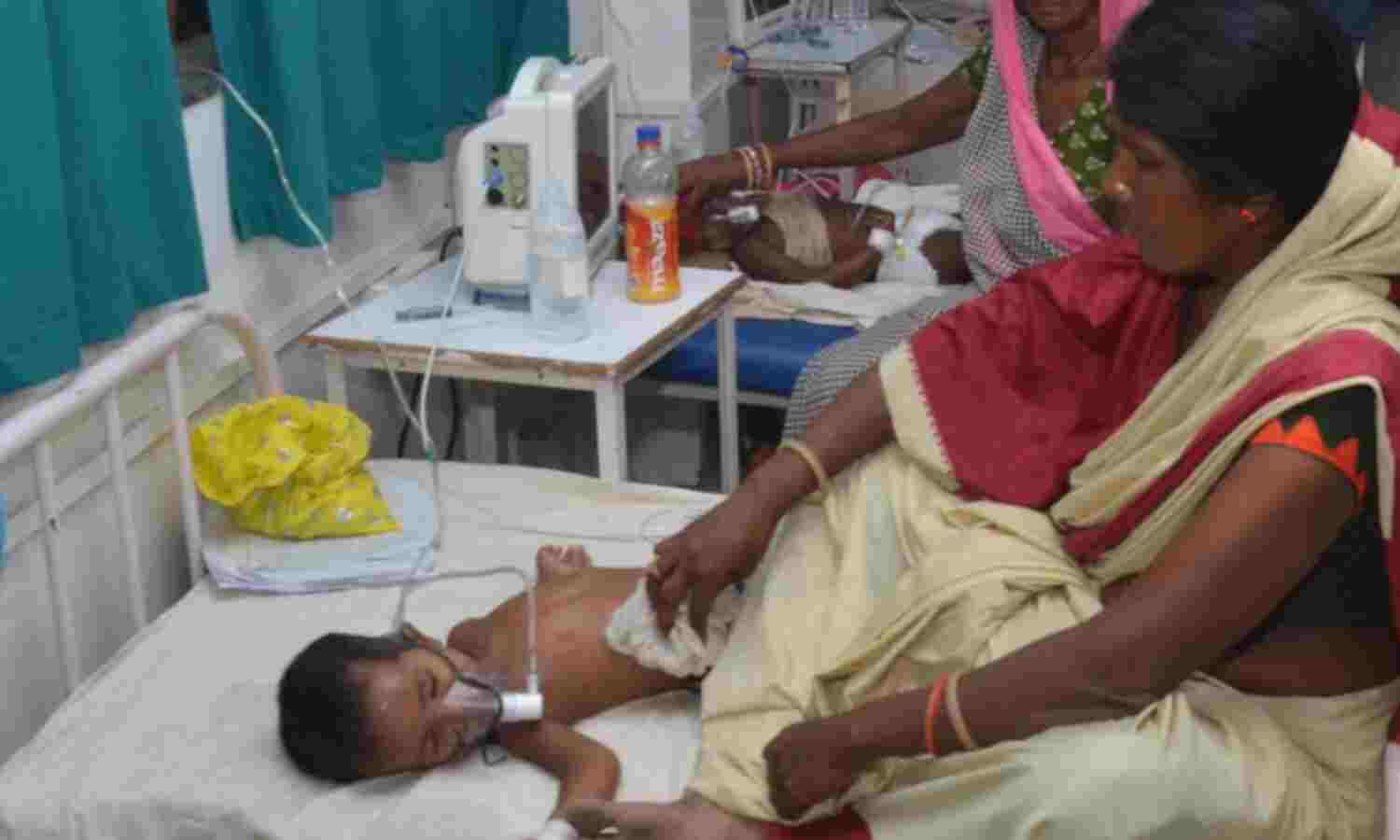
Mumbai: As Muzaffarpur, Bihar, experiences its worst encephalitis outbreak in recent history, NITI Aayog’s dashboard on state-level nutrition statistics reveals that the state ranks high in the proportion of children who are stunted (have short height for age), wasted (weigh less than normal for their height) and underweight (have low weight for their age)--the three indicators of child nutrition.
In Bihar, 48% of all children under five years are stunted, 21% are wasted, and 44% are underweight, placing the state in the first, 10th and second ranks for these three deficiencies respectively, among all 29 states in India. These figures are also either at or above the all-India average of 38%, 21% and 36%, respectively.
After Bihar, Uttar Pradesh has the highest proportion of stunted children at 46%, followed by Jharkhand (45%), Meghalaya (44%) and Madhya Pradesh (42%).
The top five states for wasting are Jharkhand (29%), Gujarat (26%), Karnataka (26%), Madhya Pradesh (26%) and Maharashtra (26%).
As far as underweight children are concerned, only Jharkhand (48%) is worse than Bihar, just ahead of Madhya Pradesh (43%), Uttar Pradesh (40%) and Gujarat (40%).
Bihar placed second worst on health indices that measure states’ annual health performance, which were released on June 25, 2019, by the NITI Aayog, the government’s think-tank, in collaboration with the Ministry of Health and Family Welfare and the World Bank. Bihar’s score of 32.1 (in 2017-18) was only better than that of Uttar Pradesh (28.6) among all states, and marked a fall from its score of 38.5 in 2015-16 which was the fourth worst figure in the country after Uttar Pradesh (33.7), Rajasthan (36.8) and Nagaland (37.4).
Bihar’s neonatal mortality rate--the death rate of infants younger than one month--was stagnant at 27 per 1,000 live births during the same period, while the proportion of children with low weight at birth (less than 2.5 kg) increased from 7.2% to 9.2%. The mortality rate among children younger than five years did improve from 48 to 43 per 1,000 live births, but fertility rate (average number of children born to a woman) “remained high” while increasing from 3.2 in 2015 to 3.3 in 2016.
Muzaffarpur not among India’s top nutrition-deficient districts
Muzaffarpur, the district that reported the deaths of 132 children due to encephalitis as of June 26, 2019, does not feature among the top districts for nutrition deficiency in India. Yet, it has 48% stunted, 18% wasted and 42% underweight children--comparable to Bihar’s figures (48%, 21% and 44%).
“Child undernutrition is caused by inadequacies in food, health and care for infants and young children, especially in the first two years of life,” said the 2015-16 district nutrition profile of Muzaffarpur collated by research group POSHAN, which ‘aims to reduce the nutrition evidence gap in India by synthesising, generating, and mobilising nutrition evidence’. “At the household and community level, women’s status, household food security, hygiene and socio-economic conditions further contribute to children’s nutrition outcomes.”
The profile noted that only 29% of pregnant women made an antenatal care (ANC) visit during their first trimester even though 85% of them had a Mother and Child Protection Card, and just 11% made at least four ANC visits, against the eight recommended by a World Health Organization study. Further, only 55% of children in the district received full immunisation during 2015-16 (against a state average of 90%), which is guaranteed to all infants and pregnant women under the government’s Universal Immunisation Programme.
Malnutrition tied to social conditions in Muzaffarpur
“Muzaffarpur is emblematic of a hot spot for undernutrition in India,” said this report on The Wire. “Children here appear to be born and grow up malnourished.”
“Although most infants are breastfed and exclusive breastfeeding is high [in the district], other aspects of infant diets are abysmal and childhood illness is high,” the report said, “Other social determinants of malnutrition--early marriage, poverty, open defecation and more--offer a case study in what one could call a ‘perfect storm’ of risk factors.”
“Poverty is a big issue there,” a development worker in Bihar, who did not wish to be named, said. “Government programmes are plentiful but implementation is a problem. There is nobody doing home visits and LBW [low birth weight] records are misreported. Women are suffering from anaemia and weakness. Moreover, quality of preventive care is very poor. Other than that, there is no particular reason why it [encephalitis] struck Muzaffarpur; it is very regular in Begusarai [another district in Bihar]. Lack of awareness is another major concern.”
Failure of government programmes
Muzaffarpur district is home to 3,801 anganwadis--child care centres instituted under the Integrated Child Development Services (ICDS) programme--according to district data on the ICDS website.
“The anganwadis could play a critical role as a social and nutrition safety net,” said The Wire report. “The supplementary nutrition programme in Bihar has been beleaguered with various challenges for years now too, unfortunately, and it is worth taking a close look at that as well.”
“Anganwadis are unable to deliver on their functions,” the development worker said. “They need more capacity, quality of training needs to improve, and workers--mostly voluntary--need to be motivated. On paper, AWCs [anganwadi centres] are functioning; in reality, they are performing poorly.”
“Everybody is blaming the government,” said Ravikant Singh, founder of humanitarian organisation Doctors For You. “ICDS should also take responsibility. But it needs further strengthening too, in terms of infrastructure and services.”
Some anganwadis were doing “very well”, another social worker, who also did not wish to be named, said, adding, “We should look at the whole ecosystem--the family… ICDS is only one of the stakeholders and can only provide supplementary help; it is the family that provides food and nutrition. Bihar is a largely rural state with livelihood dependent on the agrarian sector.”
Bihar’s poor ICDS infrastructure featured in a March 2018 IndiaSpend story, which found that “quality services provided to the beneficiaries were seriously compromised as basic amenities like toilet, drinking water, kitchen, utensils, etc. in anganwadi centres were missing”. A single anganwadi in the state was providing supplementary nutrition to 193 children in 2014, nearly three times the national average of 68 children per centre.
States with “high fertility and high population… it’s likely they need more ICDS centres, and more financing to ensure full-scale delivery of all services,” this March 2019 IndiaSpend story suggested.
This story was first published here on HealthCheck.
(Saha, an MSc student at the Symbiosis School of Economics, Pune, is an intern with IndiaSpend.)
We welcome feedback. Please write to respond@indiaspend.org. We reserve the right to edit responses for language and grammar.


